 Bunions (hallux valgus) are often described as a bump on the side of the big toe. But a bunion is more than that. The visible bump actually reflects changes in the bony framework of the front part of the foot. With a bunion, the big toe leans toward the second toe, rather than pointing straight ahead. This throws the bones out of alignment, producing the bunion's "bump." Bunions are a progressive disorder. They begin with a leaning of the big toe, gradually changing the angle of the bones over the years and slowly producing the characteristic bump, which continues to become increasingly prominent. Bunions can be painful, but not always. Bunions are always progressive, so the deformity becomes more prounced over time, even if its not painful.
Bunions (hallux valgus) are often described as a bump on the side of the big toe. But a bunion is more than that. The visible bump actually reflects changes in the bony framework of the front part of the foot. With a bunion, the big toe leans toward the second toe, rather than pointing straight ahead. This throws the bones out of alignment, producing the bunion's "bump." Bunions are a progressive disorder. They begin with a leaning of the big toe, gradually changing the angle of the bones over the years and slowly producing the characteristic bump, which continues to become increasingly prominent. Bunions can be painful, but not always. Bunions are always progressive, so the deformity becomes more prounced over time, even if its not painful. Causes
There are many factors which can contribute to the development of a bunion. The common causes are genetic factors, poor foot mechanics, high-heeled or narrow footwear and trauma to the toe. It is believed that constant stress on the joint of the big toe causes mild displacement of the bones and the joint, along with thickening of the tissues and a change in the pull of the muscles. This can result in a degree of arthritis of the joint, and over time, further displacement of the toe. This may lead to pain, difficultly with fitting shoes and corns/calloused lesions due to excess pressure on the smaller digits.
Symptoms
The skin over your big toe may be red and tender. Wearing any type of shoe may be painful. This joint flexes with every step you take. Your big toe may angle toward your second toe, or even move all the way under it. The skin on the bottom of your foot may become thicker and painful. Pressure from your big toe may force your second toe out of alignment, sometimes overlapping your third toe. If this condition gets severe, it may be difficult to walk. Your pain may become chronic and you may develop arthritis.
Diagnosis
Your doctor will be able to diagnose a bunion by asking about your symptoms and examining your feet. You may also have blood tests to rule out any other medical conditions, such as rheumatoid arthritis or gout, although this is rare. Your doctor may refer you to a podiatrist or chiropodist (healthcare professionals who specialise in conditions that affect the feet).
Non Surgical Treatment
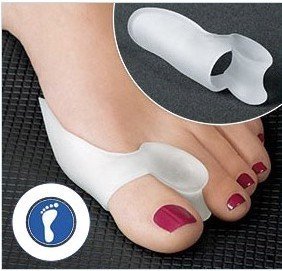
A range of treatments is available for bunions, including painkillers, modifying footwear, orthotics, such as insoles, bunion pads and toe spacers. Surgery may be considered if a person's symptoms are severe and do not respond to non-surgical treatment. The type of surgery used will depend on the level of deformity, the severity of any other associated symptoms, the patient's age and any other associated medical conditions. Bunion surgery is usually effective, with up to 85% of cases resulting in improvement to symptoms. However, the deformity can sometimes return after bunion surgery.
Surgical Treatment
Procedures are designed and chosen to correct a variety of pathologies that may be associated with the bunion. For instance, procedures may address some combination of removing the abnormal bony enlargement of the first metatarsal, realigning the first metatarsal bone relative to the adjacent metatarsal bone, straightening the great toe relative to the first metatarsal and adjacent toes, realigning the cartilagenous surfaces of the great toe joint, addressing arthritic changes associated with the great toe joint, repositioning the sesamoid bones beneath the first metatarsal bone, shortening, lengthening, raising, or lowering the first metatarsal bone, and correcting any abnormal bowing or misalignment within the great toe. Connecting two parallel long bones side by side by Syndesmosis Procedure. At present there are many different bunion surgeries for different effects. The age, health, lifestyle and activity level of the patient may also play a role in the choice of procedure. Traditional bunion surgery can be performed under local, spinal or general anesthetic. In the case of laser surgery, a narcotic analgesic is typically used.[5] The trend has moved strongly toward using the less invasive local anesthesia over the years. A patient can expect a 6- to 8-week recovery period during which crutches are usually required for aid in mobility. An orthopedic cast is much less common today as newer, more stable procedures and better forms of fixation (stabilizing the bone with screws and other hardware) are used. Hardware may even include absorbable pins that perform their function and are then broken down by the body over the course of months.